Discovery holds hope for combating gum inflammation
Scientists have determined the main causes of gingivitis, an inflammation of the gums attributed to bacterial infection which is a major cause of tooth loss in adults.
If left untreated, the bacterial infection may lead to periodontitis, a serious gum disease that damages the soft tissues around the teeth, destroying the bone that supports them.
The new findings have come following clinical investigations of saliva samples from 30 people with healthy gums and 30 with gingivitis which are reported in journal BMC Oral Health.
The authors say that according to their clinical examination the presence of MIF or Macrophage migration inhibitory factor, a protein crucial for the regulation of innate immunity, can be used by dentists as an “effective indicator” of gingivitis.
“During clinical examination, we recorded three parameters of gum health: Bleeding on probing (BOP), Visible Plaque Index (VPI), and Simplified Modified Gingival Index (SMGI). Then, we used special tests (ELISA) to measure the levels of MAF, MCF, and MIF in their saliva sample.”
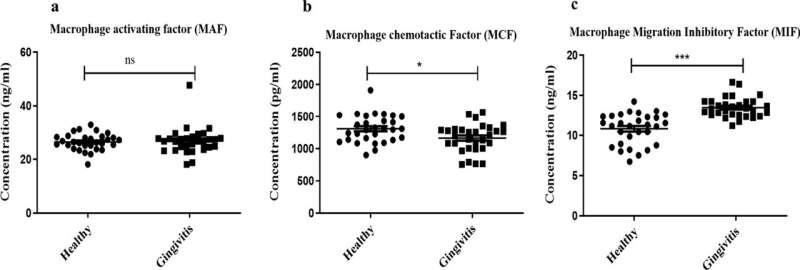
“Our findings showed that MAF levels were similar in both healthy (people) and patients with gingivitis. However, MCF and MIF levels were notably higher in those with gingivitis. Interestingly, MIF levels changed at different stages of gum inflammation. Hence our study suggests that the levels of MCF and MIF in saliva could be signs of gum inflammation. Moreover, MIF level in saliva can be used as effective indicator of gingivitis,” says co-author Prof. Sausan Al Kawas of the University of Sharjah in the United Arab Emirates (UAE).
Dr. Betul Rahman, also a co-author and an associate professor at University of Sharjah’s College of Dental Medicine, says the study records three parameters of gum health of the participants taking part in the clinical trials.
“We recorded three parameters of gum health: Bleeding on probing (BOP), Visible Plaque Index (VPI), and Simplified Modified Gingival Index (SMGI). Then, we used special tests (ELISA) to measure the levels of MAF, MCF, and MIF in their saliva sample,” adds Dr. Rahman.
The clinical investigations were done at the University Dental Hospital Sharjah from February 2020 to June 2021. Of the methods employed and the data gathered, the scientists write, “Sixty participants, 30 healthy individuals, and 30 gingivitis patients, age range between 18 and 45 years, were enrolled in this research. A verbal and written information were provided to the participants before study enrollment and informed consent was obtained from them.
“Sixty saliva specimens were collected from periodontally healthy (n = 30), and gingivitis patients (n = 30). Bleeding on probing (BOP), Visible Plaque Index (VPI), and Simplified Modified Gingival Index (SMGI) were recorded through clinical examination.
“Statistical analysis was performed using SPSS (version 28). Total mean score for each biomarker was determined, and descriptive bivariate statistics were conducted to characterize the levels of biomarkers among the study groups.”
Dr. Rahman is optimistic about the results. She says, “Our study signifies a promising step towards non-invasive diagnostics in oral health. Identifying salivary biomarkers such as MIF could revolutionize how we detect and manage gingivitis, offering a more precise and timely approach to oral care.”
The study signals fresh hope on the path of combating gingivitis, according to Prof. Kawas, who adds, “Understanding the role of macrophage-related chemokines in gingivitis is pivotal. Our findings pave the way for future research and innovations in diagnostics and therapeutic strategies for periodontal diseases.”
The study assumes added significance when taking the high prevalence of gingivitis into account and how the most common type of the gum inflammation can turn into a chronic disease. Medical literature shows that gingivitis afflicts 9-17% of children aged 3–11 years with the rate skyrocketing to 70–90% among adults.
The authors’ aim was to investigate if certain substances in saliva could shed light on gum health. “We focused on three substances in saliva—macrophage-activating factor (MAF), macrophage-chemotactic factor (MCF), and macrophage migration inhibitory factor (MIF). We looked at people with healthy gums and those with gum inflammation (gingivitis) to see if the levels of these substances were linked to how severe the gum diseases were,” says Prof. Kawas.
For long clinicians have been looking for a faster and simple non-invasive test with high accuracy as an indicator (biomarker) of gum diseases since current diagnosis methods to show bone loss and then treat gum disease have relied on things like bleeding during probing (BOP), plaque scores, clinical attachment loss, probing pocket depth, and X-rays.
However, says Dr. Rahman, these methods “are time consuming, expensive and their accuracy depends on the skills of the dentist. Saliva is the best non-invasive body fluid to use for diagnosis of many body and oral diseases. This study could be used to develop such simple and accurate test using saliva sample to diagnose and follow up on patients with gum diseases.”
The study’s findings, according to Prof. Kawas, “could potentially interest various pharmaceutical sectors related to oral health. The identification of salivary biomarkers opens avenues for the development of innovative diagnostic tools and therapeutic interventions, which could attract interest from dental care providers, diagnostic companies, and pharmaceutical organizations.
“The ultimate aim was to contribute to the development of non-invasive diagnostic tools for early detection and monitoring of gingivitis, thereby enhancing the precision of preventive and therapeutic interventions in oral health. By identifying reliable salivary biomarkers, we aimed to address the limitations of current diagnostic methods and facilitate early intervention in oral diseases.”
The authors believe that their research holds significant practical implications for the field of oral health given that the current diagnostic methods for gingivitis rely on clinical examinations, which may have limitations in identifying individuals at risk of developing periodontitis.
“Our findings suggest that salivary MIF levels could serve as a potential early diagnostic biomarker for gingivitis. This has practical implications for dental practitioners, as incorporating salivary biomarkers into routine screenings could enable more accurate and timely identification of individuals at risk. Early detection allows for timely intervention, potentially preventing the progression of gingivitis to more severe periodontal conditions,” adds Dr. Rahman.
More information:
Amna Alhammadi et al, Salivary macrophage chemokines as potential biomarkers of gingivitis, BMC Oral Health (2023). DOI: 10.1186/s12903-023-02787-5
University of Sharjah
Citation:
Physical traits of gingivitis identified: Discovery holds hope for combating gum inflammation (2024, January 29)
retrieved 29 January 2024
from https://medicalxpress.com/news/2024-01-physical-traits-gingivitis-discovery-combating.html
This document is subject to copyright. Apart from any fair dealing for the purpose of private study or research, no
part may be reproduced without the written permission. The content is provided for information purposes only.
_______
Source : medicalxpress.com